driving down the a/g index by receiving stakeholder engagement
THE CHALLENGE
A community hospital with 211 beds in the Southeast encountered various significant challenges that led to a prolonged length of stay, surpassing both internal hospital targets and industry benchmarks. While stakeholders showed a reasonable level of involvement, and interdisciplinary rounds were being conducted, the absence of a proper organizational framework hindered their overall effectiveness. Regrettably, there was no cohesive initiative in place to tackle the issues of extended length of stay and patient satisfaction.
THE SOLUTION
Core Clinical Partners initiated its intervention in December and January with multiple onsite visits by clinical and operational leaders. These visits focused on establishing relationships with the nursing staff, fostering open communication, and understanding the hospital’s specific needs through discussions with the hospital leadership.
Recruitment and Re-engagement
Significant recruiting endeavors in 2022 resulted in welcoming a number of new graduates. With new team members and refreshed leadership, including a new Medical Director, Core was able to create a renewed culture.
Core Clinical Partners, the Medical Director, nursing leadership, and hospital administrators jointly formulated an action plan to set the improvement process in motion.
Structuring Interdisciplinary Rounds (IDR)
Along with the staffing overhaul, the interdisciplinary rounds were reformatted to be scripted and precisely structured. Every patient’s identity, room number, current status, estimated discharge date, next level of care, and one-sentence plan summary were outlined, making the rounds more effective at identifying patients ready for discharge and resolving any roadblocks.
Structured Text-Blast to Improve Coordination
Core introduced a new ‘text blast’ system that used the facility’s existing technology platforms. Each morning, a text message was sent out detailing the current disposition of all inpatients expected to be discharged that day. This update preceded the late morning interdisciplinary round meeting. This system ensured that all healthcare providers were on the same page regarding patient status.
Launching Inpatient Observation
Finally, Core launched a new 14-bed inpatient observation unit operating 24/7. The medical director reviewed all observation patients, creating a paradigm shift in managing hospitalist inpatient populations. Patients who could potentially be discharged within 24 hours were grouped into their cohort, further enhancing patient management efficiency.
THE RESULT
The action taken by Core Clinical Partners led to significant improvements in the hospital’s operations:
-
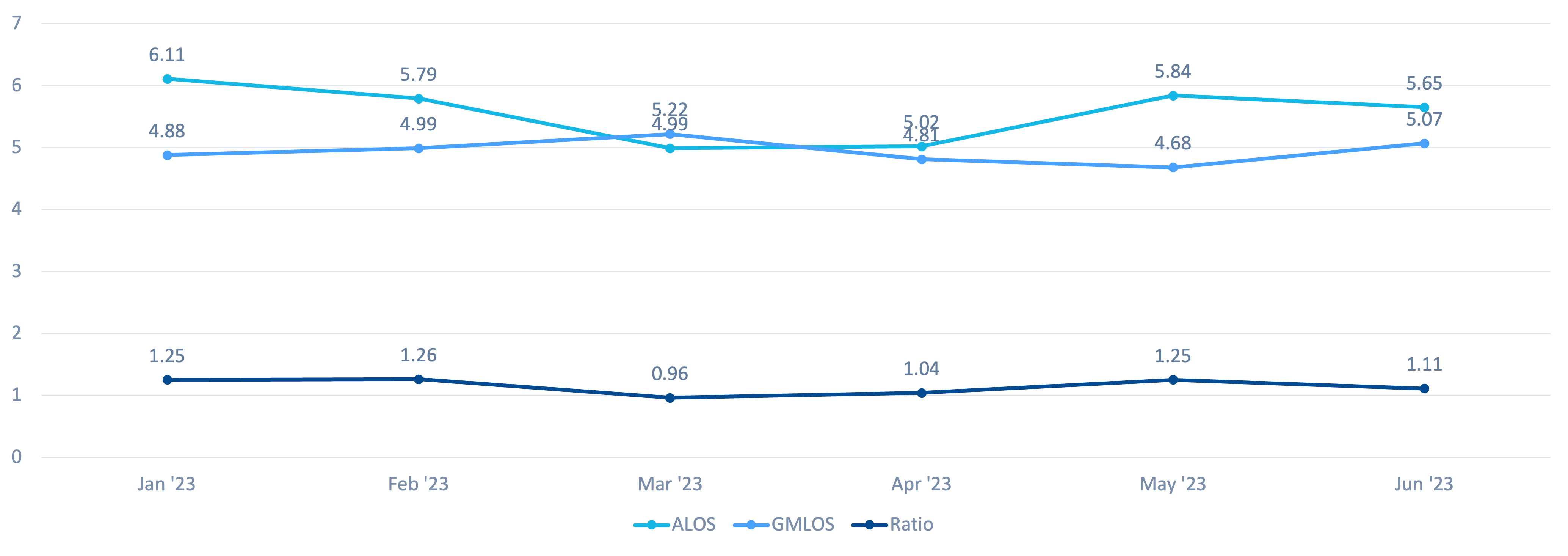
THE A/G INDEX (REPRESENTING THE AVERAGE LOS DIVIDED BY THE GEOMETRIC MEAN), DECREASED FROM A HIGH OF 1.19 BEFORE THE INITIATIVES TO CONSISTENTLY NEAR 1, THEREBY MEETING THE HOSPITAL’S GOALS.
-
THE AVERAGE LOS WAS REDUCED FROM 6.11 DAYS TO CONSISTENTLY LESS THAN 5.
-
THE MORNING ‘TEXT BLAST’ SYSTEM’S EFFICIENCY IMPROVED, WITH THE DISCHARGE ORDER GOING OUT BEFORE 11AM MORE THAN HALF THE TIME. PREVIOUSLY, THIS ONLY OCCURRED 37% OF THE TIME.
-
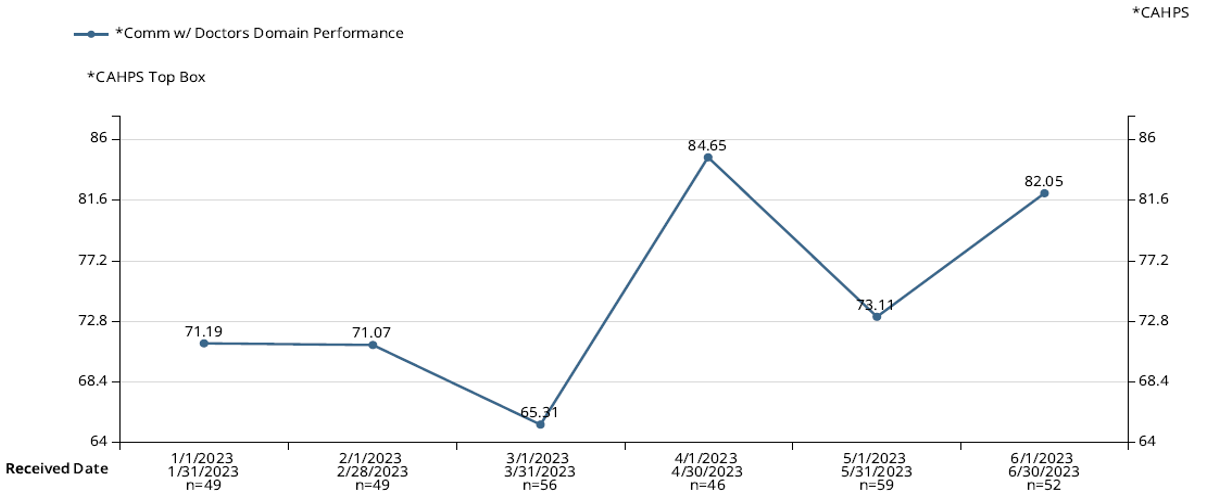
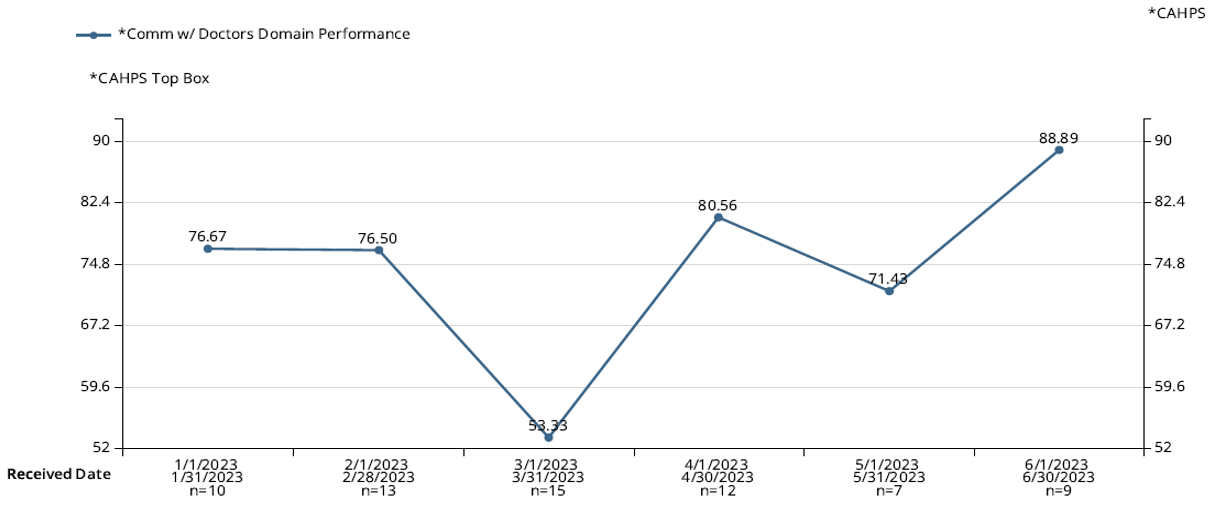
SHORTER HOSPITAL STAYS AND IMPROVED COMMUNICATION FROM CLINICIANS AROUND DISCHARGES LED TO HIGHER PATIENT SATISFACTION ACROSS ALL LEVELS.
The reformation at this community hospital showcased how a true partnership can help hospital leaders achieve their goals for Hospitalist Medicine. The engagement levels of doctors and nursing staff significantly rose, further driving these initiatives’ success. These improvements underscore the transformative potential of flexible and strategic Hospitalist Medicine management.


 THE MORNING ‘TEXT BLAST’ SYSTEM’S EFFICIENCY IMPROVED, WITH THE DISCHARGE ORDER GOING OUT BEFORE 11AM MORE THAN HALF THE TIME. PREVIOUSLY, THIS ONLY OCCURRED 37% OF THE TIME.
THE MORNING ‘TEXT BLAST’ SYSTEM’S EFFICIENCY IMPROVED, WITH THE DISCHARGE ORDER GOING OUT BEFORE 11AM MORE THAN HALF THE TIME. PREVIOUSLY, THIS ONLY OCCURRED 37% OF THE TIME.